PTSD: National Center for PTSD
Clinician-Administered PTSD Scale for DSM-5 (CAPS-5)
Clinician-Administered PTSD Scale for DSM-5 (CAPS-5)
Description
The CAPS is the gold standard in PTSD assessment. The CAPS-5 is a 30-item structured interview that can be used to:
- Make current (past month) diagnosis of PTSD
- Make lifetime diagnosis of PTSD
- Assess PTSD symptoms over the past week
In addition to assessing the 20 DSM-5 PTSD symptoms, questions target the onset and duration of symptoms, subjective distress, impact of symptoms on social and occupational functioning, improvement in symptoms since a previous CAPS administration, overall response validity, overall PTSD severity, and specifications for the dissociative subtype (depersonalization and derealization).
For each symptom, standardized questions and probes are provided. Administration requires identification of an index traumatic event to serve as the basis for symptom inquiry. The Life Events Checklist for DSM-5 (LEC-5) is recommended in addition to the Criterion A inquiry included in the CAPS-5.
The CAPS was designed to be administered by clinicians and clinical researchers who have a working knowledge of PTSD but can also be administered by appropriately trained paraprofessionals. The full interview takes 45-60 minutes to administer.
VIDEO
What is the CAPS-5 Training Curriculum?
Learn about our 4-course training on the CAPS-5 that you can take online at your own pace.
Changes from previous CAPS for DSM-IV
Several important revisions were made to the CAPS in updating it for DSM-5:
- CAPS for DSM-IV asked respondents to endorse up to three traumatic events to keep in mind during the interview. CAPS-5 requires the identification of a single index trauma to serve as the basis of symptom inquiry.
- CAPS-5 is a 30-item questionnaire, corresponding to the DSM-5 diagnosis for PTSD. The language of the CAPS-5 reflects both changes to existing symptoms and the addition of new symptoms in DSM-5. CAPS-5 asks questions relevant to assessing the dissociative subtype of PTSD (depersonalization and derealization), but no longer includes other associated symptoms (e.g., gaps in awareness).
- As with previous versions of the CAPS, CAPS-5 symptom severity ratings are based on symptom frequency and intensity (except for amnesia and diminished interest which are based on amount and intensity). However, CAPS-5 items are rated with a single severity score in contrast to previous versions of the CAPS which required separate frequency and intensity scores.
- General instructions and scoring information are included with the CAPS-5.
Scoring
Detailed scoring information is included with the CAPS-5 and should be reviewed carefully before administering. Briefly, the assessor combines information about frequency and intensity of an item into a single severity rating. CAPS-5 total symptom severity score is calculated by summing severity scores for the 20 DSM-5 PTSD symptoms. Similarly, CAPS-5 symptom cluster severity scores are calculated by summing the individual item severity scores for symptoms corresponding to a given DSM-5 cluster: Criterion B (items 1-5); Criterion C (items 6-7); Criterion D (items 8-14); and, Criterion E (items 15-20). A symptom cluster score may also be calculated for dissociation by summing items 19 and 20.
- At least one Criterion B symptom
- At least one Criterion C symptom
- At least two Criterion D symptoms
- At least two Criterion E symptoms
- Criterion F is met (disturbance has lasted one month)
- Criterion G is met (disturbance causes either clinically significant distress or functional impairment)
Sample Item
In the past month, have you had any unwanted memories of (EVENT) while you were awake, so not counting dreams?
How does it happen that you start remembering (EVENT)?
[If not clear:] (Are these unwanted memories, or are you thinking about [EVENT] on purpose?)
How much do these memories bother you?
Are you able to put them out of your mind and think about something else?
How often have you had these memories in the past month?
Severity Rating
0. Absent: The respondent denied the problem or the respondent's report doesn't fit the DSM-5 symptom criterion.
1. Mild / subthreshold: The respondent described a problem that is consistent with the symptom criterion but isn't severe enough to be considered clinically significant. The problem doesn't satisfy the DSM-5 symptom criterion and thus doesn't count toward a PTSD diagnosis.
2. Moderate / threshold: The respondent described a clinically significant problem. The problem satisfies the DSM-5 symptom criterion and thus counts toward a PTSD diagnosis. The problem would be a target for intervention. This rating requires a minimum frequency of 2 x month or some of the time (20-30%) PLUS a minimum intensity of Clearly Present.
3. Severe / markedly elevated: The respondent described a problem that is above threshold. The problem is difficult to manage and at times overwhelming, and would be a prominent target for intervention. This rating requires a minimum frequency of 2 x week or much of the time (50-60%) PLUS a minimum intensity of Pronounced.
4. Extreme / incapacitating: The respondent described a dramatic symptom, far above threshold. The problem is pervasive, unmanageable, and overwhelming, and would be a high-priority target for intervention.
Versions
There are three versions of the CAPS-5 corresponding to different time periods: past week, past month, and worst month (lifetime). The past week version of the CAPS-5 should be used only to evaluate PTSD symptoms over the past week. PTSD diagnostic status should be evaluated with the past month (for current PTSD) or worst month (for lifetime PTSD) versions of the CAPS-5.
A version for children and adolescents ages 7 and above (CAPS-CA-5) is also available. The CAPS-CA-5 corresponds to DSM-5.
Citation
Weathers, F.W., Blake, D.D., Schnurr, P.P., Kaloupek, D.G., Marx, B.P., & Keane, T.M. (2013). The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5). [Assessment] Available from www.ptsd.va.gov.
References (CAPS-5)
Marx, B. P., Lee, D. J., Norman, S. B., Bovin, M. J., Sloan, D. M., Weathers, F. W., Keane, T. M., & Schnurr, P. P. (2021). Reliable and clinically significant change in the Clinician-Administered PTSD Scale for DSM-5 and PTSD Checklist for DSM-5 among male Veterans. Psychological Assessment, Advance online publication. https://doi.org/10.1037/pas0001098
Weathers, F. W., Bovin, M. J., Lee, D. J., Sloan, D. M., Schnurr, P. P., Kaloupek, D. G., Keane, T. M., & Marx, B. P. (2018). The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5): Development and initial psychometric evaluation in military Veterans. Psychological Assessment, 30(3), 383-395. https://doi.org/10.1037/pas0000486
References (CAPS for DSM-IV)
Blake, D. D., Weathers, F. W., Nagy, L. M., Kaloupek, D. G., Gusman, F. D., Charney, D. S., & Keane, T. M. (1995). The development of a clinician-administered PTSD scale. Journal of Traumatic Stress, 8(1), 75-90. https://doi.org/10.1002/jts.2490080106
Gray, M., Litz, B., Hsu, J., & Lombardo, T. (2004). Psychometric properties of the Life Events Checklist. Assessment, 11(4), 330-341. https://doi.org/10.1177/1073191104269954
Weathers, F. W., Keane, T. M., & Davidson, J. R. (2001). Clinician-Administered PTSD Scale: A review of the first ten years of research. Depression and Anxiety, 13, 132-156. https://doi.org/10.1002/da.1029
Weathers, F. W., Ruscio, A. M., & Keane, T. M. (1999). Psychometric properties of nine scoring rules for the Clinician-Administered Posttraumatic Stress Disorder Scale. Psychological Assessment, 11(2), 124-133. https://doi.org/10.1037//1040-3590.11.2.124
Additional Reviews (CAPS for DSM-IV)
Orsillo (2001) (PDF) p. 259.
Orsillo, Susan M. (2001). Measures for acute stress disorder and posttraumatic stress disorder. In M.M. Antony & S.M. Orsillo (Eds.), Practitioner's guide to empirically based measures of anxiety (pp. 255-307). Kluwer Academic/Plenum. PTSDpubs ID 24368
CAPS-5 Training
The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5) Clinician Training offers clinicians, trainees and researchers a comprehensive review of the CAPS-5 assessment and its administration.
CONTINUING EDUCATION
Clinician-Administered PTSD Scale for DSM-5 (CAPS-5) Clinician Training
This series of online courses offers a comprehensive review of the CAPS-5 measure and its administration.
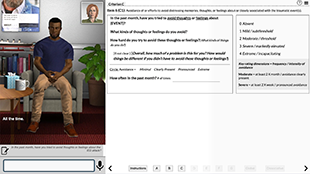
Part 1 explains the history, rationale, administration and scoring of the CAPS-5. Parts 2 through 4 are interactive online courses. They include a virtual patient who responds to prompts in real-time and on-screen coaching. Through the use of the simulator, providers and researchers learn how to administer and score the Clinician-Administered PTSD Scale for DSM-5 (CAPS-5).
To Obtain Scale
The CAPS-5 measure was created by staff at VA's National Center for PTSD. To obtain the CAPS-5 Assessments:
- Non-VA providers: Please complete the online assessment request form.
- For VA employees only: Download the CAPS-5 assessment measures on the National Center for PTSD Intranet website.
NOTE: Due to changes in regulations, if you are not a VA provider and have had access granted before, you will need to resubmit the form.
Are you using this measure with U.S. Veterans or Service members?
Our PTSD Consultation Program can answer administration or scoring questions: PTSDconsult@va.gov or 866-948-7880.
Measure availability: We provide information on a variety of measures assessing trauma and PTSD. These measures are intended for use by qualified mental health professionals and researchers. Measures authored by National Center staff are available as direct downloads or by request. Measures developed outside of the National Center can be requested via contact information available on the information page for the specific measure.